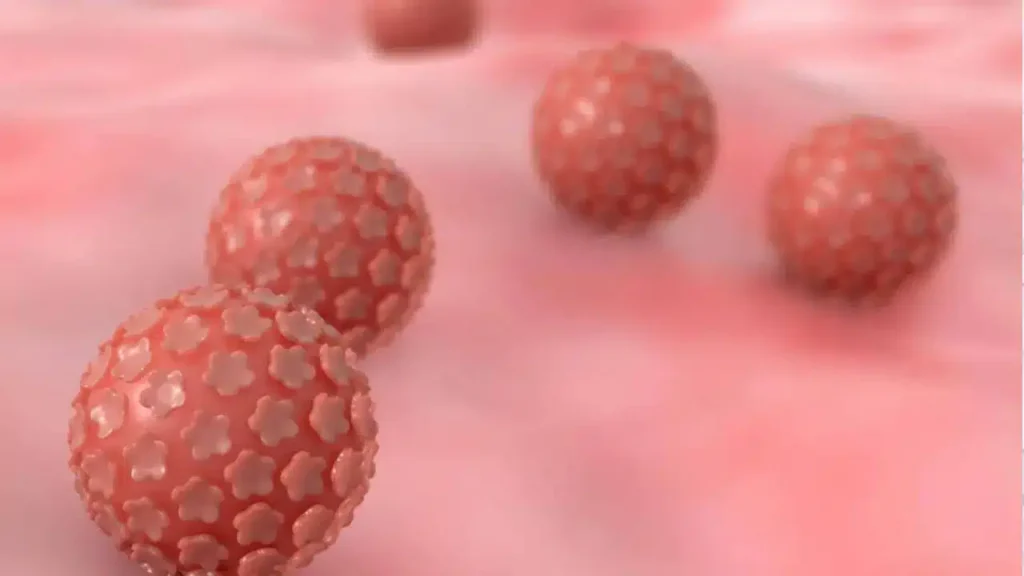
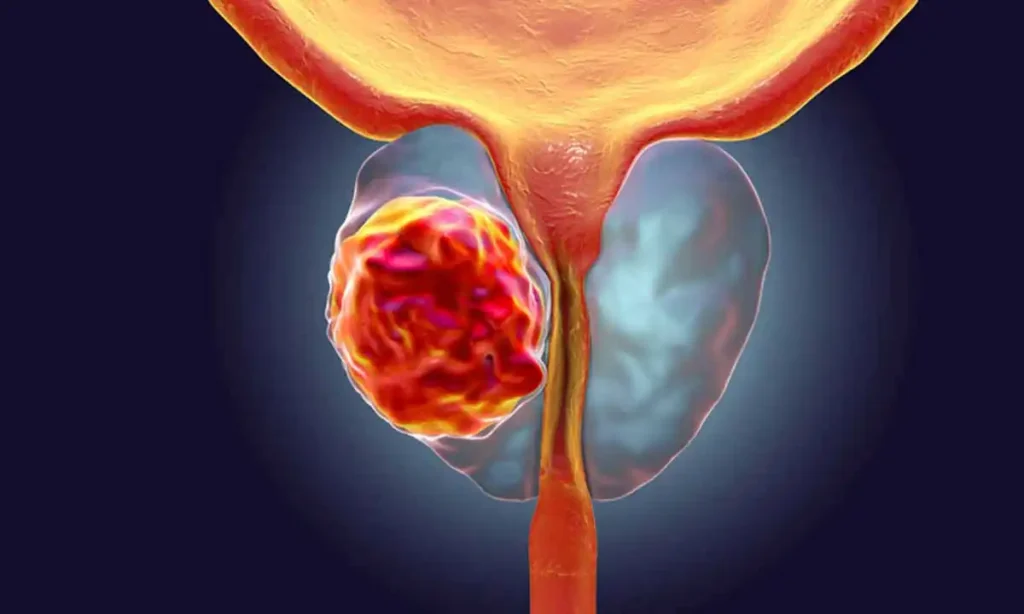
Human papillomavirus (HPV)
Human papillomavirus (HPV) is the most common sexually transmitted infection worldwide. In the United States, an estimated 14 million persons are newly infected each year [1]. Prevalence of any genital HPV is estimated at 42.5 percent among U.S. females aged 14-59 years [2]. Although most HPV infections are self-limited and cause no symptoms, persistent infections with human papillomavirus (HPV) can cause cervical and other cancers, including anal, oropharyngeal, penile, vaginal, and vulvar, as well as anogenital warts. HPV is estimated to be responsible for 40-50 percent of all invasive penile cancers and is associated with almost all cervical cancers. Cervical cancer is the second most common cancer and the fifth leading cause of death in women worldwide with nearly 4,000 dying from this disease in the U.S. each year. International Human Papillomavirus (HPV) Awareness Day falls on March 4th. The 2022 campaign theme is ” One less worry ” and focuses on three simple steps that should help in eliminating HPV – driven cancers via education (safer sex), vaccination, and early screening to detect the HPV infection. Ninety percent of genital warts are caused by HPV types 6 and 11. However, most HPV-associated cancers are caused by HPV types 16 and 18, including 15,000 cases of these cancers in females and 7,000 cases in males each year in the U.S [3]. For men, there is an overall annual increase in HPV – related cancers of 2.36 % per year, which is attributable in part to the numbers of HPV associated cancers among individuals infected with human immunodeficiency virus in high – income countries on account of the substantial incidence of anal cancer among men. Penile cancers are diagnosed more likely to be HPV – positive in recent years [4,5,6]. Penile cancer is one of the cancers that is increasing in incidence and the only such cancer that urologists manage in their clinical practice. Although rare in developed countries, as with any HPV – driven cancer, penile cancer is much more prevalent in the lowest – income countries (many of which are in sub – Saharan Africa and Latin America) [6,7]. Infections with HPV types 16, 18, 31, and 33 have been reported in high percentages of penile squamous cell carcinoma (SCC) cases, and in total it is estimated that one in two penile cancers globally is HPV-positive [7,8]. Oral HPV is associated with oropharyngeal carcinomas approximately 22.4 %, 4.4 % and 3.5 % of oral cavity, oropharynx and larynx cancers, respectively are attributed to HPV [9]. Systematic reviews have reported prevalence rates of oral HPV from 5.5-7.7 %, with HPV16 present in 1-1.4 % of patients. Risk factors for HPV infection include early age of first sexual intercourse, sexual promiscuity, higher frequency of sexual intercourse, smoking and poor immune function [10]. Overall, the prevalence of HPV in different sites seems to be higher in young, sexual – active adults compared to other population groups [10]. Stable sexual habits, circumcision and condom use are protective factors against HPV [11,12]. Added risk factors of oral HPV infection are alcohol consumption, poor oral hygiene and sexual behaviours (oral and vaginal) [10]. Positive HIV status, phimosis, and HPV status of the partner have also been associated with anogenital HPV status and decreased clearance in a number of studies [13]. HPV typically spreads by sustained direct skin – to – skin or mucosal contact, with vaginal, oral and anal sex being the most common transmission route [14]. In addition, HPV has been found on surfaces in medical settings and public environments raising the possibility of object – to – skin / mucosa transmission [15]. Further studies on non-sexual and non – penetrative sexual transmission are needed to understand the complexity of HPV transmission. HPV transmission may also be influenced by genotype, with a higher incidence of HPV51 and HPV52 and a high prevalence of HPV16 and HPV18 in the general and high – risk male population [14]. HPV presence is dependent on study setting. In men attending urological clinics HPV was detected in 6 % of urine samples [16]. A meta – analysis reported seminal HPV in 4.5-15.2 % of patients resulting in seminal HPV being associated with decreased male fertility [17]. A cross sectional study of 430 men presenting for fertility treatment detected HPV in 14.9 % of semen samples. The presence of HPV in semen was not associated with impaired semen quality [18]. However, another systematic review reported a possible association between HPV and altered semen parameters, and in women possible miscarriage or premature rupture of the membrane during pregnancy. The symptoms of HPV-infection may appear as warts on the female or male patient in equal ratio. The lesions may be large and grossly visible or may be discovered only after appropriate application of acetic acid and magnified scanning of the genitalia. In women, a screening study revealed a 2 % incidence of subclinical HPV infection in those with abnormal findings on Papanicolaou smear [19]. Any symptomatic or asymptomatic abnormal – appearing warts or lesions may be found to carry HPV infection in the external genitalia, and this can be discovered under magnification with genotype diagnosis through PCR-swabs from lesions or from condylomata warts [20]. In males, the HPV virus has been seen in warts when assessed with PCR-swabs for genotype diagnosis. Other studies have reported HPV type 16 in penile carcinoma along with types 31 and 35 [21]. The lesions may present in two basic morphologic forms. The classic wart known as condyloma acuminata presents as a verrucous papillary growth in the genital region that may range from 2 mm up to several centimeters in size. These warts may be found on the penis, perineum, or scrotum, or within the urethra. In women, the introitus, perineum, vagina, and urethra are common sites as is with the cervix. In patients who are immune suppressed, such as renal transplant recipients or patients on chemotherapy, lesions may attain enormous size and cover the entire perineum. The incidence of genital warts in children has increased
Human papillomavirus (HPV) قراءة المزيد »