Renal Cell Carcinoma
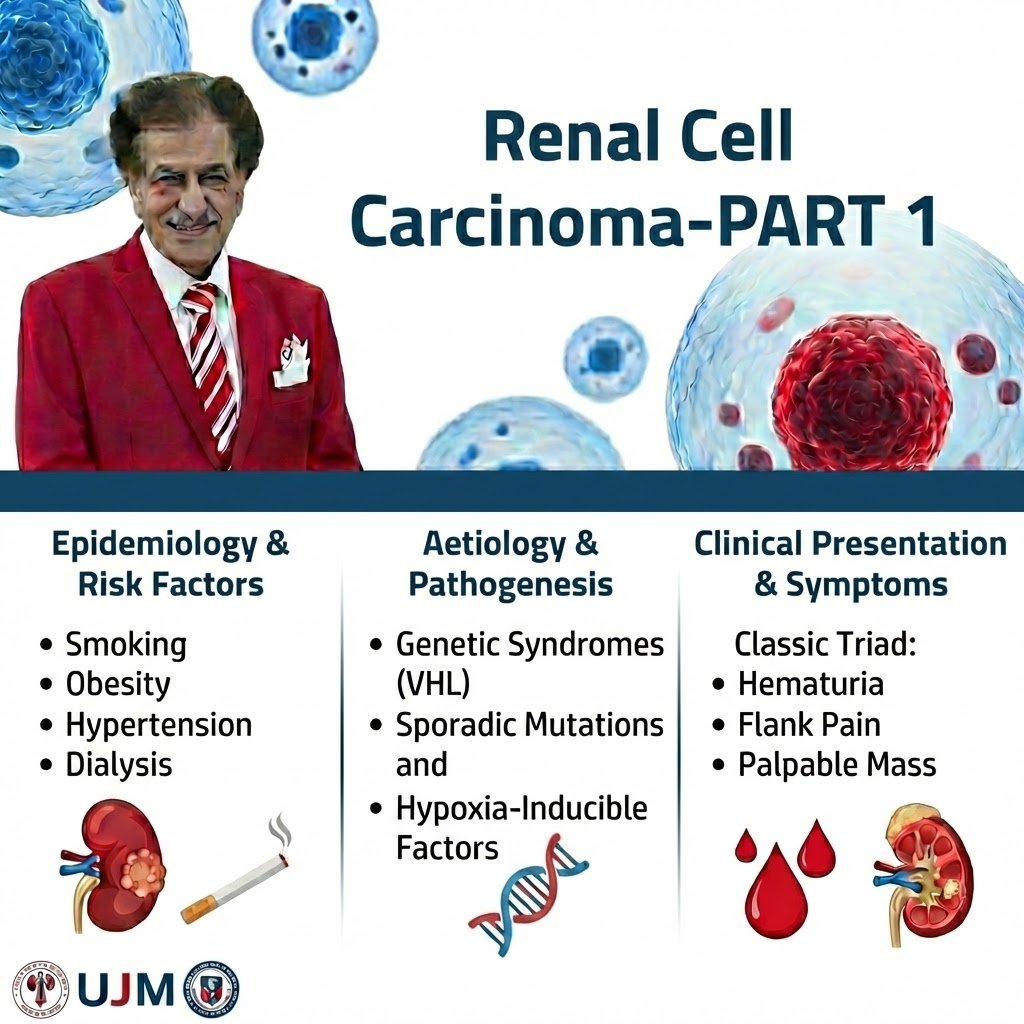
Renal Cell Carcinoma Part 1 Comprehensive Review Article Prof. Dr. Semir. A. Salim. Al Samarrai EPIDEMIOLOGY, AETIOLOGY AND PATHOLOGY: Epidemiology Renal cell carcinoma represents around 3% of all cancers, with the highest incidence occurring in Western countries [1,2]. In Europe, and worldwide, the highest incidence rates are found in the Czech Republic and Lithuania [2]. Generally, during the last two decades until recently, there has been an annual increase of about 2% in incidence both worldwide and in Europe leading to approximately 99,200 new RCC cases and 39,100 kidney cancer-related deaths within the European Union in 2018 [1,2]. In Europe, overall mortality rates for RCC increased until the early 1990s, with rates generally stabilising or declining thereafter [3]. There has been a decrease in mortality since the 1980s in Scandinavian countries and since the early 1990s in France, Germany, Austria, the Netherlands, and Italy. However, in some European countries (Croatia, Estonia, Greece, Ireland, Slovakia), mortality rates still show an upward trend [1,2]. Renal cell carcinoma is the most common solid lesion within the kidney and accounts for approximately 90% of all kidney malignancies. It comprises different RCC subtypes with specific histopathological and genetic characteristics [4]. There is a 1.5:1 predominance in men over women with a higher incidence in the older population [2,5]. Aetiology Established risk factors include lifestyle factors such as (hazard ratio [HR]: 1.23-1.58), obesity (HR 1.71), BMI (> 35 vs. < 25), and hypertension (HR: 1.70) [2,5]. 50.2% of patients with RCC are current or former smokers. By histology, the proportions of current or former smokers range from 38% in patients with chromophobe carcinoma to 61.9% in those with collecting duct/medullary carcinoma [6]. In a recent systematic review diabetes was also found to be detrimental [7]. Having a first-degree relative with kidney cancer is also associated with an increased risk of RCC. Moderate alcohol consumption appears to have a protective effect for reasons as yet unknown, while any physical activity level also seems to have a small protective effect [2, 7–11]. A number of other factors have been suggested to be associated with higher or lower risk of RCC, including specific dietary habits and occupational exposure to specific carcinogens, but the literature is inconclusive [5]. The most effective prophylaxis is to avoid cigarette smoking and reduce obesity [2,5]. Histological Diagnosis diagnosis Strong Renal cell carcinomas comprise a broad spectrum of histopathological entities described in the 2016 World Health Organization (WHO) classification [4]. There are three main RCC types: clear cell (ccRCC), papillary (pRCC type I and II) and chromophobe (chRCC). The RCC type classification has been confirmed by cytogenetic and genetic analyses [4,12]. Histological diagnosis includes, besides RCC type; evaluation of nuclear grade, sarcomatoid features, vascular invasion, tumour necrosis, and invasion of the collecting system and peri-renal fat, pT, or even pN categories. The four-tiered WHO/ISUP (International Society of Urological Pathology) grading system has replaced the Fuhrman grading system [4]. Clear-cell RCC Overall, clear-cell RCC (ccRCC) is well circumscribed and a capsule is usually absent. The cut surface is golden-yellow, often with haemorrhage and necrosis. Loss of chromosome 3p and mutation of the von HippelLindau (VHL) gene at chromosome 3p25 are frequently found. The loss of von Hippel-Lindau protein function contributes to tumour initiation, progression, and metastases. The 3p locus harbours at least four additional ccRCC tumour suppressor genes (UTX, JARID1C, SETD2, PBRM1) [12]. In general, ccRCC has a worse prognosis compared to pRCC and chRCC, but this difference disappears after adjustment for stage and grade [13,14]. Papillary RCC Papillary RCC is the second most commonly encountered morphotype of RCC. Papillary RCC has traditionally been subdivided into two types [4]. Type I and II pRCC, which were shown to be clinically and biologically distinct; pRCC type I is associated with activating germline mutations of MET and pRCC type II is associated with activation of the NRF2-ARE pathway and at least three subtypes [15]. Type II pRCC presents a heterogenous group of tumours and future substratification is expected, e.g., oncocytic pRCC [4]. A typical histology of pRCC type I (narrow papillae without any binding, and only microcapillaries in papillae) explains its typical clinical signs. Narrow papillae without any binding and a tough pseudocapsule explain the ideal rounded shape (Pascal’s law) and fragility (specimens have a “minced meat” structure). Tumour growth causes necrotisation of papillae, which is a source of hyperosmotic proteins that cause subsequent “growth” of the tumour, fluid inside the tumour, and only a serpiginous, contrast-enhancing margin. Stagnation in the microcapillaries explain the minimal post-contrast attenuation on CT. Papillary RCC type 1 can imitate a pathologically changed cyst (Bosniak IIF or III). The typical signs of pRCC type 1 are as follows: an ochre colour, more frequently exophytic, extrarenal growth, low grade, and low malignant potential; over 75% of these tumours can be treated by NSS surgery. A substantial risk of renal tumour biopsy tract seeding exists (12.5%), probably due to the fragility of the tumour papillae [16]. Papillary RCC type I is more common and generally considered to have a better prognosis than pRCC type II [4, 14, 17]. Chromophobe RCC Overall, chRCC is a pale tan, relatively homogenous and tough, well-demarcated mass without a capsule. Chromophobe RCC cannot be graded by the Fuhrman grading system because of its innate nuclear atypia. An alternative grading system has been proposed, but has yet to be validated [4]. Loss of chromosomes Y, 1, 2, 6, 10, 13, 17 and 21 are typical genetic changes [4]. The prognosis is relatively good, with high fiveyear recurrence-free survival (RFS), and ten-year cancer-specific survival (CSS) [18]. The five- and ten-year recurrence-free survival rates were 94.3% and 89.2%, respectively. Recurrent disease developed in 5.7% of patients, and 76.5% presented with distant metastases with 54% of metastatic disease diagnoses involving a single organ, most commonly bone. Recurrence and death after surgically resected chRCC is rare. For completely excised lesions < pT2a without coagulative necrosis or sarcomatoid features, prognosis is excellent [19]. The new WHO/ISUP grading system merges former entity ‘hybrid oncocytic chromophobe tumour’
Renal Cell Carcinoma قراءة المزيد »